I have to plead guilty to having completely neglected this blog since late August. I think you'll understand. As you might guess from my nom de blog, I live in New Orleans. We lost our house and Katrina and everything has been chaos since. More of that story in my house blog.
One of the many lessons learned these months with regard to Susan, is just how important early intervention really is. Susan has gotten physical therapy, occupational therapy, and special instruction since she was six months old. I've always described it to people as "nice girls coming over the play with the baby." As she has gotten older, the therapy has become more intensive. She does things in PT that I could never do, like sitting up against gravity on an exercise ball. After we'd been in Houston for a couple of days, I contacted the Texas Early Childhood Intervention program to get Susan in their system, because we didn't know when or if we might be going back to Louisiana and I didn't want her to lose months of therapy.
I totally have my hat off to Texas and the people of Houston in particular. They got Susan into the program without all of the standard medical records and referrals, and waived the usual parental copay for treatments, because of our refugee status. I don't know that Louisiana could or would have done the same. Even with their amazing helpfulness, just the process of finding service providers and scheduling appointments took us to about a month out from our arrival before Susan was able to start getting any treatments. Naturally, Mr. Nola and I work with her ourselves and try to keep her moving and active, but there is just a difference between what the parents can do and what the therapists can do. As her Mom, I'm not going to push her so hard she's unhappy. Especially during such a stressful time, I had to be her "safe place." When the PT comes in though, Susan knows it's time to work, and she cooperates much more than she would have with me.
Another issue was that our home-in-exile was not set up to be baby resistant, and if left on the floor for long, Susan could create total havoc. She found pulling books from their shelves to be especially fun, and taking CDs out of their cases was a real treat. Basically we had to hold her or keep her in the high chair to keep her from destroying the place, since it wasn't ours to destroy. During that time, we saw definite signs of backsliding, particularly in her gross motor skills. She wouldn't stand for long, or push up on her arms much, or do much of anything we had been working on in PT for months beforehand.
As soon as we started seeing the Texas PT, she was trying new things again. The PT could show us techniques to use to encourage her to sit or stand the best way to get her ready to learn the next skill. Susan also gained enough confidence to be willing to try.
Really, the biggest difference has just been getting into our own place (albeit a different place than before the storm) where we can let her make a mess and scoot about the house freely. Having carpet instead of wood floors at our apartment creates more resistance when she's scooting, so she's working harder to move around and getting stronger. I think the carpet also makes her more confident to try standing because she doesn't feel as likely to hurt herself if she falls. As much as I prefer the look of the wood floors, when/if we rebuild our house we're going to use carpet in the family room and bedrooms to make them play-friendly.
Of the four therapists she was seeing before Katrina, only one is back at work in the New Orleans area. Fortunately, we've been able to get her into the early intervention program at a local hospital, where they have their own excellent staff service providers. They are coming out to the house to see her until the end of the year, then in January she's going to start going to play group at a nearby hospital where the treatments are integrated into a nursery school program. We think having that social interaction will motivate her to want to do things she sees the other kids doing - like eat and walk.
I think the group will be great for her, once she gets settled in and comfortable there. We've had a hard time in the past with leaving her with sitters, but at least she has a chance to get to know the providers this month before the group starts. I am also delighted at the prospect of a couple of baby-free hours a week to get work or errands done. As much fun as she is, it's pretty much impossible to do anything that requires concentration while she's with me. Just while I've been typing this post, she's dismembered my wallet and spread checks and credit cards all over the living room.
Wednesday, December 14, 2005
Monday, November 21, 2005
Tuesday, November 15, 2005
Screw spammers, too
I'm turning the comments off on this account because of the annoying spam I keep getting. On the off chance any of said spammers are actually reading this, I assure you I will not be banking any cord blood because 1) I won't be having any more kids, 2) it's a scam, and 3) you piss me off. I have enough crap to deal with without your phony input.
Friday, August 26, 2005
Terrific Preemie Article
August 14, 2005
New York Times Magazine
A Second Womb
By PAUL RAEBURN
Even before Heidelise Als escorted me into the intensive-care unit for newborns at Children's Hospital in Boston, she began to whisper. Als understands, as much as anyone, that premature infants are fragile creatures and that even the smallest noise or disruption can overload their still-developing plum-size brains. Stepping gently, she led me to a tiny boy lying on his back in a plastic bed no bigger than a briefcase. He was surrounded by a tangled nest of wires, tubes and hoses, a respirator and other lifesaving devices. As we watched, a nurse arrived and fumbled with an IV needle; she grabbed one of the baby's tiny, almost translucent heels and stretched his leg in the air to give herself room to work. The baby tried to retract his leg. He started to cry.
The nurse glanced at Als and then pushed the needle into the heel. Als winced. The nurse couldn't find a vein. She pulled the other leg, tried that heel and failed again. The baby cried harder. Als cupped her hands over her mouth; she knew she shouldn't interfere, but she had trouble restraining herself. A second nurse came and put her hands on the baby's chest to keep him from squirming. Als walked away. She couldn't watch any longer.
Als, a developmental psychologist at Harvard Medical School and Children's Hospital, has spent most of her life trying to see and feel the world through the eyes, ears and fragile skin of premature babies. It is a simple idea, but a radical one. And it holds the promise of a bold and, she would add, necessary reformation of this country's care of the prematurely born.
Preemies -- babies born anywhere from a few weeks to a few months before they are due -- arrive in the world with their brains still under construction. In the last few decades, neonatal intensive-care units, or N.I.C.U.'s, have made it possible for ever more preemies to survive and prosper, often with magnificent results. But even if the infant's body appears to be functioning perfectly when the baby leaves the hospital, difficulties may still lie ahead. Despite their impressive technological sophistication, N.I.C.U.'s cannot ensure that brain maturation follows its proper course. Recent studies show that preemies are disproportionately prone to learning disabilities and psychiatric illnesses, like anxiety and attention-deficit hyperactivity disorder. The more premature the baby, the more likely the disability.
Als's proclaimed mission is to make the intensive-care unit safe for the development of the brain. In a series of innovative studies, she has shown that a gentler environment in the N.I.C.U. can alleviate many of the complications of premature birth. ''You have to watch the baby, to listen to the baby,'' she says. ''The baby is a partner in everything you do.'' Als argues that N.I.C.U.'s must become quieter, darker and more responsive to a baby's desire for comfort and movement; ultimately, they should be as reminiscent of the womb's nurturing environment as doctors and nurses can make them. She has helped to institute many of her reforms at the hospitals where she works in Boston, and she has trained a cadre of others to carry her message across the country and to Europe and South America.
Dr. T. Berry Brazelton, the noted authority on child development and a pediatrician at Children's Hospital, has known Als since the 1970's, when she came to Boston to study with him. ''She's changed the whole atmosphere of how we approach premature babies from a medical and environmental standpoint,'' he says. She has shown ''how life can be improved for them and what we can do to cut down on the medical cost and the cost for these kids' futures.''
Before birth, a fetus is an aquatic creature, bobbing in a warm, dark amniotic pool. After spending nine months bathing in the womb, it is well prepared for its exit into the world. Preemies, however, leave their mothers' bodies with vital brain wiring unfinished. In order to make sure that the wiring process is completed, they need to continue their development in as supportive an external environment as possible.
Instead, they trade the soft surroundings of maternal flesh for an alien, high-tech hospital ward where they are subjected to the most unnatural manipulations. They are poked and prodded dozens of times each day. Nurses flip them almost upside down to change their diapers, wildly altering their blood pressure. In the typical N.I.C.U., their senses are overwhelmed by ringing telephones, screeching alarms and cold fluorescent lights that burn 24 hours a day. Metal carts bang into one another as attendants cross one another's path. Als herself was surprised at how noisy some N.I.C.U.'s can be. Some of her studies require monitoring a sleeping infant's brain-wave activity with an EEG for six minutes. ''To get a six-minute quiet sleep EEG, we may have to record for three hours because of the continuous sound interruptions that arouse the baby's brain,'' she says.
Doctors and nurses in the N.I.C.U. do not aim to treat babies harshly. They are simply making sure the N.I.C.U. does what it must do: deliver oxygen, provide the babies with nutrition and save them from medical emergencies that threaten their lives. Without those essential services, the babies would not survive. But that doesn't protect them from more subtle problems. ''A large number of these babies do reasonably well and go home,'' says Tonse N.K. Raju, a specialist in newborns at the National Institute of Child Health and Human Development, part of the National Institutes of Health. ''But can we assure the family that everything is fine? The answer is no.''
Als, who is 64, moves delicately and quietly in the cloisters of the N.I.C.U., but she is forceful and direct when out of earshot of the babies. She is passionate about her dual roles as a researcher and an advocate for premature children. Born in Germany, she married an American and soon after moved to Philadelphia, where she studied developmental psychology and physical anthropology at the University of Pennsylvania. She absorbed the work of the primatologists Jane Goodall and Dian Fossey and the paleontologist Richard Leakey. She was particularly interested in how our animal ancestors cared for their children. ''We come into the world with a way of processing the world,'' she says. ''I wanted to find out where that comes from.''
While she was in graduate school, she gave birth to a son, Christopher, who was born full term. Within hours of his birth, however, it was apparent to Als that something was wrong: ''He cried from Day 1. I found myself adapting in order to get him not to cry. I learned intuitively that I had to be calm to keep him calm.'' As time went on, further problems developed. He was slow in learning to walk. He was easily overstimulated and would become agitated in response to too much activity, not unlike many premature infants. He began having seizures at age 2, and before long it became clear that he was significantly brain-damaged.
The consequences were devastating. Her marriage collapsed, and she was left to raise Christopher alone. Often, he couldn't tell her what he wanted or needed. When he spoke, she had to interpret what he said. When he didn't, she had to search his eyes and learn to read his movements. She learned to be exceedingly patient and to perceive the subtle signals she was receiving from Christopher. (Her son, now 40, lives in a community for adults with developmental disabilities, where Als and her current husband visit him often.) When Als arrived at Children's Hospital in 1973, she approached premature babies in part using the skills she learned caring for Christopher. She learned to read their subtle cues and signals and began to reimagine the N.I.C.U. from the babies' point of view.
What she saw was dismaying. In the womb, babies are vibrant, active and in constant physical and hormonal contact with their mothers. In the N.I.C.U., they're limp little bundles, lying flopped on their backs, their arms extended and eyes closed. Their noses, hands, chests or feet are often pinned with gauze and adhesive tape. And they are repeatedly stuck with needles, intravenous tubes and catheters. ''They are sustaining pain at a level that is completely unexpected,'' Als says. ''It's overwhelming to the brain.'' In today's N.I.C.U., ventilators pump bursts of pressurized air into their lungs hundreds of times per minute, making them vibrate and shiver as if they were frightened animals. ''The technologies are so advanced, yet in comparison to the womb, they are crassly primitive.''
Als would like the N.I.C.U. to mimic the womb as much as possible, but that's not easy. Before birth, the baby and the mother are locked in an intricate dance. Each affects the hormonal behavior of the other. They move together, they share the same food and they may even share some of the same feelings. Little is understood about this complicated relationship, but even as more is learned, it is very unlikely that N.I.C.U. doctors will ever perfectly recreate conditions in the uterus. They would need not only a mechanical womb but also a mechanical mother with mechanical hormones and mechanical hopes and fears. Still, anything they can do to make the intensive-care environment more baby-friendly should increase the chances for normal brain development.
Of course, not all premature children are in equal need of such measures. Some do well in the hospital and go on to lead normal lives. They develop differently from their full-term peers; it takes them a little longer to catch up. But they don't necessarily suffer any long-term effects.
There is no question, however, that premature babies, as a group, face particular risks. In a study reported in January 2005, Dr. Neil Marlow and colleagues at the Queen's Medical Center in Nottingham, England, examined 241 6-year-olds who were among the earliest surviving premature infants; they were all born more than three months premature. Only about 10 percent had serious physical disabilities. But, Marlow says: ''Just over 41 percent were scoring in the learning difficulty range. That was a lot higher that we'd predicted.'' Studies in the United States have reached similar conclusions. By age 8, one in five premature kids, on average, has repeated at least one grade in school. An even more recent study of 8-year-olds who were born weighing less than 2.2 pounds, which was published in July in The Journal of the American Medical Association, found that the children were far more likely than their full-term counterparts to have low I.Q.'s and poor academic and motor skills. These very premature babies ''fared substantially worse than [normal birthweight children] in every type of assessment,'' the journal said in a commentary.
These statistics would be troubling enough if prospective parents were fully aware of the risks of premature birth. But doctors say that many parents are not adequately prepared -- including parents undergoing in vitro fertilization, who have a higher-than-normal chance of having twins or triplets, which are more likely to be born prematurely. Hellen Russo and her husband, Anthony, of North Branford, Conn., say that they had only a limited understanding of the risks when their I.V.F. twins arrived three months premature 13 years ago. ''We had been so focused on infertility that premature babies never crossed our minds,'' she says. Before their twin boys, Anthony and Michael, were born, Russo and her husband say that they learned little from their doctors about what the long-term consequences of their early births might be. The Russos' doctors did what they were trained to do: they overcame the life-threatening complications in the N.I.C.U. and saved the children.
In the years since, the Russo twins have experienced a variety of complications. At age 3, Michael and Anthony went to a public preschool program for children with learning difficulties. Michael, who had a nearly fatal stroke in the N.I.C.U., is weak on his left side and walks with a slight limp. Anthony has a less severe weakness on his right side. He limps a little, and his handwriting -- he is right-handed -- is a little jagged. Both tried playing hockey, but neither was able to balance well enough on skates. Anthony had reading problems in kindergarten and first grade. ''He couldn't read as quickly as the other children, and he couldn't keep up, especially if it involved writing,'' his mother says. Michael has had more serious problems. While he has become an enthusiastic baseball and basketball player, ''he's not focused,'' she says. ''His attention span is poor. He's lazy, and he has no interest in school.'' Russo says that she didn't anticipate any of this when she brought the boys home from the hospital. ''You think once you've got them out of the newborn nursery and you get them home,'' she continues, ''things will be fine.''
Researchers don't know precisely how the intensive-care unit interferes with proper brain development. Premature children could be missing vital nutrients or growth factors that they get in the womb. Or their development could be disrupted by the unnatural environment of the N.I.C.U.
Inside the uterus, Als explains, babies develop their sense of touch in constant contact with warm, gently swirling fluid. In that nearly weightless environment, they can easily curl up and lift their hands to their mouths. That sets up feedback loops in the brain -- ''the brain grows from that,'' Als explains. The child is in constant communication with its mother. ''Her rhythms, her eating, her happiness, her upset, all those hormones in her own makeup transmit themselves to the fetus through the umbilical cord,'' she says. ''The fetus is tuned into his environment. It tastes and smells the fluid all the time. For 40 weeks, it's tasting its mother.'' By the time of birth, the full-term baby has developed sensory filters that allow it to tune out certain sounds and sensations, just as adults tune out other people's conversations in a crowded room. That way, it can focus its attention on the voice and touch of its mother.
When a baby comes into the world prematurely, those filters are not in place. Suddenly it sees light, form and color. It smells soap and disinfectant. It loses its amniotic bath. ''It's moved abruptly from being an aquatic animal to a terrestrial animal, and it's stuck on a flat surface,'' Als says. It can no longer curl forward easily. Many premature babies, active and toned when they are born, lose that tone within days and become unresponsive. Their unnatural environment almost certainly contributes to the brain-related problems that preterm children develop, Als says.
Als has devised a palette of techniques that offer at least a partial solution to these problems. She has turned down the lights while still leaving enough light to work and to see when the babies are in trouble. When the lights are lower, doctors and nurses talk more quietly, for the same reason that a dimly lighted restaurant is usually quieter than a diner. ''Everyone simmers down,'' Als says. ''We know that when we talk about 'mood lighting.'''
She has instructed nurses to surround babies with a ''nest'' of blankets. In the womb, babies' skin registers the constant pressure of amniotic fluid. The nest provides an approximation of that all-surrounding sense of touch. The nest can't be too tight; the baby needs room to move, she says. When babies have to fight to move, they quickly tire, part of the reason they become limp and unresponsive.
Als has encouraged nurses and doctors to change their basic procedures from the moment of the baby's arrival. ''When a baby is born, everybody works to get at him'' in the N.I.C.U., says Sandra Harmon, the assistant nurse manager in the N.I.C.U. at Brigham and Women's Hospital in Boston. That can include a nurse, triage doctor, intern, one or more residents, a fellow, the attending physician and a respiratory therapist. ''They're all trying to do their thing around this little baby, who might weigh only a pound,'' Harmon says. The N.I.C.U's at Brigham and Women's and Children's hospitals now limit the number of people who converge on a new arrival.
Als also encourages N.I.C.U. doctors and nurses to ensure that the babies experience long periods of near-complete darkness. At Children's Hospital, when doctors or nurses aren't working with a baby, the baby's incubator is covered with a blanket to give it a chance to sleep. Als has explained to her colleagues that the babies are far more aware of their surroundings than the doctors and nurses had thought. When she and I toured the N.I.C.U., she made that point for me by gingerly lifting the corner of one of the blankets. The baby inside the incubator reacted immediately -- his breathing became less stable and he shifted his position, even though he hadn't opened his eyes. ''He knows we're peeking,'' she said.
In 2003, Als and a dozen colleagues reported on the effectiveness of a treatment program that requires doctors and nurses to deliver food and care on a schedule that gives the infants more time to rest, relax and sleep. The care was organized around the needs of the individual infants and families, instead of the work schedules of the doctors and nurses. The findings were remarkable. The babies moved more quickly from intravenous to oral feeding. They spent less time in the N.I.C.U. and had fewer infections, better motor skills and a better ability to focus their attention. They grew faster. And their families displayed less stress and had better relationships with their children. The study provided ''clear evidence for the effectiveness of individualized developmental care,'' the researchers concluded.
In a follow-up study last year, Als and her team studied the brain development of premature kids and found further evidence of enhanced brain function and structure in children in the individualized program. There were more neural connections, and those connections more closely paralleled the wiring that would have developed if the babies had remained in the womb for nine months.
One reason for the success of these programs was the training of nurses and doctors and the offering of support for parents, Als says. She and her colleagues have devised a training program that is now offered by nine centers in the United States, four in Europe and one in Argentina.
Even with these successes, Als says that she has fallen short of her goals. Ultimately, she would like to take a radical step: eliminate the incubator altogether. ''My dream is a womb room for each baby and each family.'' That is, each family would be given a room of its own, with controlled temperature, humidity and oxygen. The mother would receive her postpartum care there; she and the rest of the family would live in the womb room until the baby was ready to go home. Als may not know how to recreate the aquatic environment inside the mother's body, but in a womb room the mother could at least hold the baby against her skin, where it would feel her heartbeat. ''For many people, it's a big, big step even to envision this. I don't think it's unrealistic,'' she says.
Als's efforts to reform the N.I.C.U. come at a critical time, when premature births are taking place more frequently. The decision by many women to wait until later in life to have children, and their growing reliance on fertility treatments, increases the chances that their children will arrive early. Of the 4 million babies born in this country each year, some 500,000 are born after spending 37 weeks or fewer in the womb -- a 29 percent rise since 1981.
Doctors have also vastly improved their technologies for keeping preemies alive. In the 1970's, fewer than 20 percent of newborns weighing less than 2.2 pounds -- approximately three months premature -- survived. In the three decades since then, improvements in the technology have boosted the survival rate to 70 percent, and it is even higher for babies born closer to term. (For unknown reasons, girls do a little better than boys.) In rare cases, doctors are saving even smaller babies, who would have had no chance only a few years ago. In September 2004, for example, a Chicago woman gave birth to a baby girl weighing only 8.6 ounces: she was small enough to curl up inside a toddler's slipper. Dr. Jonathan Muraskas, a neonatal specialist at Loyola University Medical Center near Chicago, was convinced that he could save the girl. She was discharged on Feb. 8, weighing 5 pounds 8 ounces -- more than 10 times what she weighed when she was born five months earlier.
These improvements in care have been a blessing. But an unintended consequence is that growing numbers of children with cognitive and psychiatric problems are being delivered to hospitals, preschools and elementary schools that don't have the resources to care for them. Als's work could change that, reducing the burden on schools and hospitals and easing the financial and emotional toll on families.
Thus far, parents, who might seem to be Als's natural allies, have not been demanding better care for their premature infants. Few realize that N.I.C.U.'s are not what they could be, and even fewer are aware of Als's own work. Muraskas, whose success with tiny babies has excited the public, worries that ''miracle newborns,'' as he calls them, ''raise false expectations for families, caregivers and the medical-legal community.'' He cites one study in which researchers followed a single infant for three months in an intensive-care unit and found that it received help from 483 different people. ''With so many people communicating with families, it is not surprising the families are confused,'' he says.
Not all the news is bleak, even for preemies who are not being treated with the Als techniques. Dr. Laura R. Ment, a professor of pediatrics and neurology at Yale University School of Medicine, has monitored 500 premature children as part of a continuing study of the consequences of prematurity. Almost 60 percent of the children showed improvement in cognitive function. Their I.Q. scores bubble upward, lifting some into the normal range. The improvements have been greatest in two-parent families, in families with more highly educated mothers and in children whose mothers received special services, like assistance with physical therapy and speech therapy for their children. The findings are encouraging. The brains of these children are still growing, and they can recover, at least partly, from the circumstances of their births.
Jerome Kagan, a Harvard University psychologist who has studied children for 40 years, underscores the point about the importance of a good home in improving the outlook for premature infants. Children born only slightly premature show little extra risk of cognitive troubles -- if they are raised by competent, caring parents. The problems tend to be more severe in homes where children aren't properly cared for. ''If you're mildly premature and you're raised in a home in poverty where nobody's talking to you and you're not being cared for, the data show you don't do as well in school,'' he says.
Als has also emphasized the importance of listening to the parents as well as the babies. Brazelton, the author of many parenting books, including the best-selling ''Touchpoints,'' about the emotional and behavioral development of children, agrees: ''If the parents take a baby like this home and treat him or her as if it's a failure, it will be a self-fulfilling prophecy.'' Brazelton notes that his first grandchild, a boy, was born almost three months premature. He's now 20. ''He's 6-feet-3,'' Brazelton says, ''and he's brilliant.''
Als is planning further, larger studies on the consequences of improved care for preemies. And she is still asking preemies what they want. ''The baby is our guide,'' she says. ''Can we read your behavior well enough to see how far away you are from being comfortable? And what can we do to help you get there?''
She visits the N.I.C.U. regularly to remind herself of what her work is about. And because she wants to be with the babies, to listen to them. ''I always feel extremely humble,'' she says, ''when I go in there, when I think about how little we know -- and how much more that baby wants of us.''
Paul Raeburn is the author, most recently, of ''Acquainted With the Night,'' a memoir of raising children who have depression and bipolar disorder. It has just been published in paperback.
Copyright 2005 The New York Times Company
New York Times Magazine
A Second Womb
By PAUL RAEBURN
Even before Heidelise Als escorted me into the intensive-care unit for newborns at Children's Hospital in Boston, she began to whisper. Als understands, as much as anyone, that premature infants are fragile creatures and that even the smallest noise or disruption can overload their still-developing plum-size brains. Stepping gently, she led me to a tiny boy lying on his back in a plastic bed no bigger than a briefcase. He was surrounded by a tangled nest of wires, tubes and hoses, a respirator and other lifesaving devices. As we watched, a nurse arrived and fumbled with an IV needle; she grabbed one of the baby's tiny, almost translucent heels and stretched his leg in the air to give herself room to work. The baby tried to retract his leg. He started to cry.
The nurse glanced at Als and then pushed the needle into the heel. Als winced. The nurse couldn't find a vein. She pulled the other leg, tried that heel and failed again. The baby cried harder. Als cupped her hands over her mouth; she knew she shouldn't interfere, but she had trouble restraining herself. A second nurse came and put her hands on the baby's chest to keep him from squirming. Als walked away. She couldn't watch any longer.
Als, a developmental psychologist at Harvard Medical School and Children's Hospital, has spent most of her life trying to see and feel the world through the eyes, ears and fragile skin of premature babies. It is a simple idea, but a radical one. And it holds the promise of a bold and, she would add, necessary reformation of this country's care of the prematurely born.
Preemies -- babies born anywhere from a few weeks to a few months before they are due -- arrive in the world with their brains still under construction. In the last few decades, neonatal intensive-care units, or N.I.C.U.'s, have made it possible for ever more preemies to survive and prosper, often with magnificent results. But even if the infant's body appears to be functioning perfectly when the baby leaves the hospital, difficulties may still lie ahead. Despite their impressive technological sophistication, N.I.C.U.'s cannot ensure that brain maturation follows its proper course. Recent studies show that preemies are disproportionately prone to learning disabilities and psychiatric illnesses, like anxiety and attention-deficit hyperactivity disorder. The more premature the baby, the more likely the disability.
Als's proclaimed mission is to make the intensive-care unit safe for the development of the brain. In a series of innovative studies, she has shown that a gentler environment in the N.I.C.U. can alleviate many of the complications of premature birth. ''You have to watch the baby, to listen to the baby,'' she says. ''The baby is a partner in everything you do.'' Als argues that N.I.C.U.'s must become quieter, darker and more responsive to a baby's desire for comfort and movement; ultimately, they should be as reminiscent of the womb's nurturing environment as doctors and nurses can make them. She has helped to institute many of her reforms at the hospitals where she works in Boston, and she has trained a cadre of others to carry her message across the country and to Europe and South America.
Dr. T. Berry Brazelton, the noted authority on child development and a pediatrician at Children's Hospital, has known Als since the 1970's, when she came to Boston to study with him. ''She's changed the whole atmosphere of how we approach premature babies from a medical and environmental standpoint,'' he says. She has shown ''how life can be improved for them and what we can do to cut down on the medical cost and the cost for these kids' futures.''
Before birth, a fetus is an aquatic creature, bobbing in a warm, dark amniotic pool. After spending nine months bathing in the womb, it is well prepared for its exit into the world. Preemies, however, leave their mothers' bodies with vital brain wiring unfinished. In order to make sure that the wiring process is completed, they need to continue their development in as supportive an external environment as possible.
Instead, they trade the soft surroundings of maternal flesh for an alien, high-tech hospital ward where they are subjected to the most unnatural manipulations. They are poked and prodded dozens of times each day. Nurses flip them almost upside down to change their diapers, wildly altering their blood pressure. In the typical N.I.C.U., their senses are overwhelmed by ringing telephones, screeching alarms and cold fluorescent lights that burn 24 hours a day. Metal carts bang into one another as attendants cross one another's path. Als herself was surprised at how noisy some N.I.C.U.'s can be. Some of her studies require monitoring a sleeping infant's brain-wave activity with an EEG for six minutes. ''To get a six-minute quiet sleep EEG, we may have to record for three hours because of the continuous sound interruptions that arouse the baby's brain,'' she says.
Doctors and nurses in the N.I.C.U. do not aim to treat babies harshly. They are simply making sure the N.I.C.U. does what it must do: deliver oxygen, provide the babies with nutrition and save them from medical emergencies that threaten their lives. Without those essential services, the babies would not survive. But that doesn't protect them from more subtle problems. ''A large number of these babies do reasonably well and go home,'' says Tonse N.K. Raju, a specialist in newborns at the National Institute of Child Health and Human Development, part of the National Institutes of Health. ''But can we assure the family that everything is fine? The answer is no.''
Als, who is 64, moves delicately and quietly in the cloisters of the N.I.C.U., but she is forceful and direct when out of earshot of the babies. She is passionate about her dual roles as a researcher and an advocate for premature children. Born in Germany, she married an American and soon after moved to Philadelphia, where she studied developmental psychology and physical anthropology at the University of Pennsylvania. She absorbed the work of the primatologists Jane Goodall and Dian Fossey and the paleontologist Richard Leakey. She was particularly interested in how our animal ancestors cared for their children. ''We come into the world with a way of processing the world,'' she says. ''I wanted to find out where that comes from.''
While she was in graduate school, she gave birth to a son, Christopher, who was born full term. Within hours of his birth, however, it was apparent to Als that something was wrong: ''He cried from Day 1. I found myself adapting in order to get him not to cry. I learned intuitively that I had to be calm to keep him calm.'' As time went on, further problems developed. He was slow in learning to walk. He was easily overstimulated and would become agitated in response to too much activity, not unlike many premature infants. He began having seizures at age 2, and before long it became clear that he was significantly brain-damaged.
The consequences were devastating. Her marriage collapsed, and she was left to raise Christopher alone. Often, he couldn't tell her what he wanted or needed. When he spoke, she had to interpret what he said. When he didn't, she had to search his eyes and learn to read his movements. She learned to be exceedingly patient and to perceive the subtle signals she was receiving from Christopher. (Her son, now 40, lives in a community for adults with developmental disabilities, where Als and her current husband visit him often.) When Als arrived at Children's Hospital in 1973, she approached premature babies in part using the skills she learned caring for Christopher. She learned to read their subtle cues and signals and began to reimagine the N.I.C.U. from the babies' point of view.
What she saw was dismaying. In the womb, babies are vibrant, active and in constant physical and hormonal contact with their mothers. In the N.I.C.U., they're limp little bundles, lying flopped on their backs, their arms extended and eyes closed. Their noses, hands, chests or feet are often pinned with gauze and adhesive tape. And they are repeatedly stuck with needles, intravenous tubes and catheters. ''They are sustaining pain at a level that is completely unexpected,'' Als says. ''It's overwhelming to the brain.'' In today's N.I.C.U., ventilators pump bursts of pressurized air into their lungs hundreds of times per minute, making them vibrate and shiver as if they were frightened animals. ''The technologies are so advanced, yet in comparison to the womb, they are crassly primitive.''
Als would like the N.I.C.U. to mimic the womb as much as possible, but that's not easy. Before birth, the baby and the mother are locked in an intricate dance. Each affects the hormonal behavior of the other. They move together, they share the same food and they may even share some of the same feelings. Little is understood about this complicated relationship, but even as more is learned, it is very unlikely that N.I.C.U. doctors will ever perfectly recreate conditions in the uterus. They would need not only a mechanical womb but also a mechanical mother with mechanical hormones and mechanical hopes and fears. Still, anything they can do to make the intensive-care environment more baby-friendly should increase the chances for normal brain development.
Of course, not all premature children are in equal need of such measures. Some do well in the hospital and go on to lead normal lives. They develop differently from their full-term peers; it takes them a little longer to catch up. But they don't necessarily suffer any long-term effects.
There is no question, however, that premature babies, as a group, face particular risks. In a study reported in January 2005, Dr. Neil Marlow and colleagues at the Queen's Medical Center in Nottingham, England, examined 241 6-year-olds who were among the earliest surviving premature infants; they were all born more than three months premature. Only about 10 percent had serious physical disabilities. But, Marlow says: ''Just over 41 percent were scoring in the learning difficulty range. That was a lot higher that we'd predicted.'' Studies in the United States have reached similar conclusions. By age 8, one in five premature kids, on average, has repeated at least one grade in school. An even more recent study of 8-year-olds who were born weighing less than 2.2 pounds, which was published in July in The Journal of the American Medical Association, found that the children were far more likely than their full-term counterparts to have low I.Q.'s and poor academic and motor skills. These very premature babies ''fared substantially worse than [normal birthweight children] in every type of assessment,'' the journal said in a commentary.
These statistics would be troubling enough if prospective parents were fully aware of the risks of premature birth. But doctors say that many parents are not adequately prepared -- including parents undergoing in vitro fertilization, who have a higher-than-normal chance of having twins or triplets, which are more likely to be born prematurely. Hellen Russo and her husband, Anthony, of North Branford, Conn., say that they had only a limited understanding of the risks when their I.V.F. twins arrived three months premature 13 years ago. ''We had been so focused on infertility that premature babies never crossed our minds,'' she says. Before their twin boys, Anthony and Michael, were born, Russo and her husband say that they learned little from their doctors about what the long-term consequences of their early births might be. The Russos' doctors did what they were trained to do: they overcame the life-threatening complications in the N.I.C.U. and saved the children.
In the years since, the Russo twins have experienced a variety of complications. At age 3, Michael and Anthony went to a public preschool program for children with learning difficulties. Michael, who had a nearly fatal stroke in the N.I.C.U., is weak on his left side and walks with a slight limp. Anthony has a less severe weakness on his right side. He limps a little, and his handwriting -- he is right-handed -- is a little jagged. Both tried playing hockey, but neither was able to balance well enough on skates. Anthony had reading problems in kindergarten and first grade. ''He couldn't read as quickly as the other children, and he couldn't keep up, especially if it involved writing,'' his mother says. Michael has had more serious problems. While he has become an enthusiastic baseball and basketball player, ''he's not focused,'' she says. ''His attention span is poor. He's lazy, and he has no interest in school.'' Russo says that she didn't anticipate any of this when she brought the boys home from the hospital. ''You think once you've got them out of the newborn nursery and you get them home,'' she continues, ''things will be fine.''
Researchers don't know precisely how the intensive-care unit interferes with proper brain development. Premature children could be missing vital nutrients or growth factors that they get in the womb. Or their development could be disrupted by the unnatural environment of the N.I.C.U.
Inside the uterus, Als explains, babies develop their sense of touch in constant contact with warm, gently swirling fluid. In that nearly weightless environment, they can easily curl up and lift their hands to their mouths. That sets up feedback loops in the brain -- ''the brain grows from that,'' Als explains. The child is in constant communication with its mother. ''Her rhythms, her eating, her happiness, her upset, all those hormones in her own makeup transmit themselves to the fetus through the umbilical cord,'' she says. ''The fetus is tuned into his environment. It tastes and smells the fluid all the time. For 40 weeks, it's tasting its mother.'' By the time of birth, the full-term baby has developed sensory filters that allow it to tune out certain sounds and sensations, just as adults tune out other people's conversations in a crowded room. That way, it can focus its attention on the voice and touch of its mother.
When a baby comes into the world prematurely, those filters are not in place. Suddenly it sees light, form and color. It smells soap and disinfectant. It loses its amniotic bath. ''It's moved abruptly from being an aquatic animal to a terrestrial animal, and it's stuck on a flat surface,'' Als says. It can no longer curl forward easily. Many premature babies, active and toned when they are born, lose that tone within days and become unresponsive. Their unnatural environment almost certainly contributes to the brain-related problems that preterm children develop, Als says.
Als has devised a palette of techniques that offer at least a partial solution to these problems. She has turned down the lights while still leaving enough light to work and to see when the babies are in trouble. When the lights are lower, doctors and nurses talk more quietly, for the same reason that a dimly lighted restaurant is usually quieter than a diner. ''Everyone simmers down,'' Als says. ''We know that when we talk about 'mood lighting.'''
She has instructed nurses to surround babies with a ''nest'' of blankets. In the womb, babies' skin registers the constant pressure of amniotic fluid. The nest provides an approximation of that all-surrounding sense of touch. The nest can't be too tight; the baby needs room to move, she says. When babies have to fight to move, they quickly tire, part of the reason they become limp and unresponsive.
Als has encouraged nurses and doctors to change their basic procedures from the moment of the baby's arrival. ''When a baby is born, everybody works to get at him'' in the N.I.C.U., says Sandra Harmon, the assistant nurse manager in the N.I.C.U. at Brigham and Women's Hospital in Boston. That can include a nurse, triage doctor, intern, one or more residents, a fellow, the attending physician and a respiratory therapist. ''They're all trying to do their thing around this little baby, who might weigh only a pound,'' Harmon says. The N.I.C.U's at Brigham and Women's and Children's hospitals now limit the number of people who converge on a new arrival.
Als also encourages N.I.C.U. doctors and nurses to ensure that the babies experience long periods of near-complete darkness. At Children's Hospital, when doctors or nurses aren't working with a baby, the baby's incubator is covered with a blanket to give it a chance to sleep. Als has explained to her colleagues that the babies are far more aware of their surroundings than the doctors and nurses had thought. When she and I toured the N.I.C.U., she made that point for me by gingerly lifting the corner of one of the blankets. The baby inside the incubator reacted immediately -- his breathing became less stable and he shifted his position, even though he hadn't opened his eyes. ''He knows we're peeking,'' she said.
In 2003, Als and a dozen colleagues reported on the effectiveness of a treatment program that requires doctors and nurses to deliver food and care on a schedule that gives the infants more time to rest, relax and sleep. The care was organized around the needs of the individual infants and families, instead of the work schedules of the doctors and nurses. The findings were remarkable. The babies moved more quickly from intravenous to oral feeding. They spent less time in the N.I.C.U. and had fewer infections, better motor skills and a better ability to focus their attention. They grew faster. And their families displayed less stress and had better relationships with their children. The study provided ''clear evidence for the effectiveness of individualized developmental care,'' the researchers concluded.
In a follow-up study last year, Als and her team studied the brain development of premature kids and found further evidence of enhanced brain function and structure in children in the individualized program. There were more neural connections, and those connections more closely paralleled the wiring that would have developed if the babies had remained in the womb for nine months.
One reason for the success of these programs was the training of nurses and doctors and the offering of support for parents, Als says. She and her colleagues have devised a training program that is now offered by nine centers in the United States, four in Europe and one in Argentina.
Even with these successes, Als says that she has fallen short of her goals. Ultimately, she would like to take a radical step: eliminate the incubator altogether. ''My dream is a womb room for each baby and each family.'' That is, each family would be given a room of its own, with controlled temperature, humidity and oxygen. The mother would receive her postpartum care there; she and the rest of the family would live in the womb room until the baby was ready to go home. Als may not know how to recreate the aquatic environment inside the mother's body, but in a womb room the mother could at least hold the baby against her skin, where it would feel her heartbeat. ''For many people, it's a big, big step even to envision this. I don't think it's unrealistic,'' she says.
Als's efforts to reform the N.I.C.U. come at a critical time, when premature births are taking place more frequently. The decision by many women to wait until later in life to have children, and their growing reliance on fertility treatments, increases the chances that their children will arrive early. Of the 4 million babies born in this country each year, some 500,000 are born after spending 37 weeks or fewer in the womb -- a 29 percent rise since 1981.
Doctors have also vastly improved their technologies for keeping preemies alive. In the 1970's, fewer than 20 percent of newborns weighing less than 2.2 pounds -- approximately three months premature -- survived. In the three decades since then, improvements in the technology have boosted the survival rate to 70 percent, and it is even higher for babies born closer to term. (For unknown reasons, girls do a little better than boys.) In rare cases, doctors are saving even smaller babies, who would have had no chance only a few years ago. In September 2004, for example, a Chicago woman gave birth to a baby girl weighing only 8.6 ounces: she was small enough to curl up inside a toddler's slipper. Dr. Jonathan Muraskas, a neonatal specialist at Loyola University Medical Center near Chicago, was convinced that he could save the girl. She was discharged on Feb. 8, weighing 5 pounds 8 ounces -- more than 10 times what she weighed when she was born five months earlier.
These improvements in care have been a blessing. But an unintended consequence is that growing numbers of children with cognitive and psychiatric problems are being delivered to hospitals, preschools and elementary schools that don't have the resources to care for them. Als's work could change that, reducing the burden on schools and hospitals and easing the financial and emotional toll on families.
Thus far, parents, who might seem to be Als's natural allies, have not been demanding better care for their premature infants. Few realize that N.I.C.U.'s are not what they could be, and even fewer are aware of Als's own work. Muraskas, whose success with tiny babies has excited the public, worries that ''miracle newborns,'' as he calls them, ''raise false expectations for families, caregivers and the medical-legal community.'' He cites one study in which researchers followed a single infant for three months in an intensive-care unit and found that it received help from 483 different people. ''With so many people communicating with families, it is not surprising the families are confused,'' he says.
Not all the news is bleak, even for preemies who are not being treated with the Als techniques. Dr. Laura R. Ment, a professor of pediatrics and neurology at Yale University School of Medicine, has monitored 500 premature children as part of a continuing study of the consequences of prematurity. Almost 60 percent of the children showed improvement in cognitive function. Their I.Q. scores bubble upward, lifting some into the normal range. The improvements have been greatest in two-parent families, in families with more highly educated mothers and in children whose mothers received special services, like assistance with physical therapy and speech therapy for their children. The findings are encouraging. The brains of these children are still growing, and they can recover, at least partly, from the circumstances of their births.
Jerome Kagan, a Harvard University psychologist who has studied children for 40 years, underscores the point about the importance of a good home in improving the outlook for premature infants. Children born only slightly premature show little extra risk of cognitive troubles -- if they are raised by competent, caring parents. The problems tend to be more severe in homes where children aren't properly cared for. ''If you're mildly premature and you're raised in a home in poverty where nobody's talking to you and you're not being cared for, the data show you don't do as well in school,'' he says.
Als has also emphasized the importance of listening to the parents as well as the babies. Brazelton, the author of many parenting books, including the best-selling ''Touchpoints,'' about the emotional and behavioral development of children, agrees: ''If the parents take a baby like this home and treat him or her as if it's a failure, it will be a self-fulfilling prophecy.'' Brazelton notes that his first grandchild, a boy, was born almost three months premature. He's now 20. ''He's 6-feet-3,'' Brazelton says, ''and he's brilliant.''
Als is planning further, larger studies on the consequences of improved care for preemies. And she is still asking preemies what they want. ''The baby is our guide,'' she says. ''Can we read your behavior well enough to see how far away you are from being comfortable? And what can we do to help you get there?''
She visits the N.I.C.U. regularly to remind herself of what her work is about. And because she wants to be with the babies, to listen to them. ''I always feel extremely humble,'' she says, ''when I go in there, when I think about how little we know -- and how much more that baby wants of us.''
Paul Raeburn is the author, most recently, of ''Acquainted With the Night,'' a memoir of raising children who have depression and bipolar disorder. It has just been published in paperback.
Copyright 2005 The New York Times Company
Thursday, August 25, 2005
New feeding plan
I'm constantly fiddling with the schedule and amount of food Susan gets through her g-tube. I can dilute or concentrate her formula for less or more calories per ounce, give lots of small feeds or fewer bigger ones, try to get most of her formula in her during the day (so she sleeps better) or during the night (so she eats better orally.) Trial and error is pretty much our only way to tell what will work best for her. Remember the game show "Press Your Luck" where the contestants would yell "big money, big money, no whammies, no whammies, STOP!" and if the spinner stopped on the evil little Whammie dude they lost their money? It's kind of like that here. "More calories, more calories, no puking, no puking, STOP!"
Over the year or so we've been playing this game, I've learned that she handles more volume of a lower calorie mix better than a smaller amount of a really concentrated formula. For reasons nobody knows, she tolerates periodic feedings better than continuous pump feeds, but I can only put so much into her at one time without her puking, so we've been doing the two ounces every hour thing for a long time now. It's very hard to keep up with that schedule, and gives her no chance to experience a fullness/hunger cycle - an important step to getting her to eat.
I was talking with the occupational therapist who teaches Susan's eating class and she said it would be really great if we could get her onto a schedule of five ounces of formula every three hours, as that would meet her caloric needs while replicating a more normal eating pattern. Right, I thought. I'd never gotten her to handle more than three and a half ounces at a time.
So, there's this button on the feeding pump that says "INT." There is no mention of this button in the instructions, nor on their website. I'd asked the equipment company if they had a pump that would do periodic rather than continuous feeds. They said they didn't carry any pumps that did that. But I started playing around with the INT button and figured out that I COULD program the pump to give her X number of ounces at Y rate every Z hours. Aha! So I played a game of press my luck, and programmed it to give five ounces over a half hour period every three hours. And what do you know, it worked.
So now I'm using the pump for her daytime feedings too, just hooking her up for the half hour every three hours. Since the pump gives a slower delivery than just dumping it down through a syringe, like I had been doing, her stomach is expanding to accommodate the higher amount. Larger volume is a huge step forward for her. Everyone cross your fingers that it continues to work.
As you can probably tell, I spend a lot of time multiplying calories and ounces and percent of formula vs percent of liquid, not to mention converting ounces to ml's, since of course the pump uses metric measure while the formula nutritional information is in English units. I'm a total math loser too, but I've got the ml's/ounce and calories/ounce thing down pretty well. Sometimes around 3 am I just give up and figure she'll get whatever calories she gets and it'll just have to be good enough.
Over the year or so we've been playing this game, I've learned that she handles more volume of a lower calorie mix better than a smaller amount of a really concentrated formula. For reasons nobody knows, she tolerates periodic feedings better than continuous pump feeds, but I can only put so much into her at one time without her puking, so we've been doing the two ounces every hour thing for a long time now. It's very hard to keep up with that schedule, and gives her no chance to experience a fullness/hunger cycle - an important step to getting her to eat.
I was talking with the occupational therapist who teaches Susan's eating class and she said it would be really great if we could get her onto a schedule of five ounces of formula every three hours, as that would meet her caloric needs while replicating a more normal eating pattern. Right, I thought. I'd never gotten her to handle more than three and a half ounces at a time.
So, there's this button on the feeding pump that says "INT." There is no mention of this button in the instructions, nor on their website. I'd asked the equipment company if they had a pump that would do periodic rather than continuous feeds. They said they didn't carry any pumps that did that. But I started playing around with the INT button and figured out that I COULD program the pump to give her X number of ounces at Y rate every Z hours. Aha! So I played a game of press my luck, and programmed it to give five ounces over a half hour period every three hours. And what do you know, it worked.
So now I'm using the pump for her daytime feedings too, just hooking her up for the half hour every three hours. Since the pump gives a slower delivery than just dumping it down through a syringe, like I had been doing, her stomach is expanding to accommodate the higher amount. Larger volume is a huge step forward for her. Everyone cross your fingers that it continues to work.
As you can probably tell, I spend a lot of time multiplying calories and ounces and percent of formula vs percent of liquid, not to mention converting ounces to ml's, since of course the pump uses metric measure while the formula nutritional information is in English units. I'm a total math loser too, but I've got the ml's/ounce and calories/ounce thing down pretty well. Sometimes around 3 am I just give up and figure she'll get whatever calories she gets and it'll just have to be good enough.
Monday, August 22, 2005
Cindy Crawford, you guilt-mongering bitch!
Over the last couple of months I've fallen into the habit of snuggling with Susan in my bed until she goes to sleep and I move her to her crib. Sometimes I just nap with her, since our night sleep is frequently interrupted and I can use the rest. But as much as I enjoy the snuggle time, she's been taking longer and longer to fall asleep, and it's impossible for anyone but me to get her down without hours of hysterical tears. So we've decided it's time to sleep-train her. In other words, we'll put her in her crib to sleep every time, and let her cry it out until she learns to go to sleep on her own.
So, I went to Barnes and Noble and picked up Healthy Sleep Habits, Happy Child by Dr. Marc Weissbluth, who is known as the go-to guy for getting babies to sleep. It has a foreward by no less an authority than supermodel Cindy Crawford. On the whole, Weissbluth has useful, important information about the sleep needs of infants and toddlers and how to help them get what they need. His delivery though, well, you be the judge. In the introduction, this is in bold print:
WARNING!
If your child does not learn to sleep well, he may become an incurable adult insomniac, chronically disabled from sleepiness and dependent on sleeping pills.
Aaaaah! My baby's going to be a drug addict because I let her nap in my bed!
This is why mothers are so stressed out. It's not enough to just feed and love our children, and provide them with a safe environment. Along with Weissbluth's book at Barnes and Noble are titles including, I kid you not, Teach your Baby to Read and How to Have a Smarter Baby. One of the babies at Susan's play group wears a bib emblazoned with the words "Future CEO" to collect his drool while he fingerpaints.
In a way, it make my life easier that Susan has some medical issues because we're officially out of the race in the Mommy/Baby competition. Other mothers feel like they have to teach their infant 50 words in sign language and all their colors and shapes by their first birthday. I'd just like Susan to learn to walk and eat in time to start nursery school when she's three. That frees me up to enjoy her company without all the mind-fuckery.
So, I went to Barnes and Noble and picked up Healthy Sleep Habits, Happy Child by Dr. Marc Weissbluth, who is known as the go-to guy for getting babies to sleep. It has a foreward by no less an authority than supermodel Cindy Crawford. On the whole, Weissbluth has useful, important information about the sleep needs of infants and toddlers and how to help them get what they need. His delivery though, well, you be the judge. In the introduction, this is in bold print:
If your child does not learn to sleep well, he may become an incurable adult insomniac, chronically disabled from sleepiness and dependent on sleeping pills.
Aaaaah! My baby's going to be a drug addict because I let her nap in my bed!
This is why mothers are so stressed out. It's not enough to just feed and love our children, and provide them with a safe environment. Along with Weissbluth's book at Barnes and Noble are titles including, I kid you not, Teach your Baby to Read and How to Have a Smarter Baby. One of the babies at Susan's play group wears a bib emblazoned with the words "Future CEO" to collect his drool while he fingerpaints.
In a way, it make my life easier that Susan has some medical issues because we're officially out of the race in the Mommy/Baby competition. Other mothers feel like they have to teach their infant 50 words in sign language and all their colors and shapes by their first birthday. I'd just like Susan to learn to walk and eat in time to start nursery school when she's three. That frees me up to enjoy her company without all the mind-fuckery.
Sunday, August 21, 2005
Honoring Susan Torres
Just about everybody who blogs about parenting has talked about Susan Torres, the 26-year-old Virginia woman who suffered a stroke while pregnant, and was kept alive on life support so that her baby would have a chance to survive.
Naturally, I've been rooting for this baby. As terrible as the family's loss is, they have Susan's last great gift to the world to remember her by. My own Susan, as well as many other preemies, are testaments to the quality of life that is possible for kids born early. So it's surprised me to see a lot of people whose opinions I respect criticize Jason Torres, Susan's husband, for keeping her alive. He's been accused of using his dead wife as an incubator, of taxing the medical system's resources for a child with poor prospects, and of neglecting his older child's needs while attending to his dying wife and nascent baby.
On the other hand, he's also being held up as a hero to the pro-life movement, and Susan it's martyr. I'm totally appalled that people are using this family's tragedy to highlight their political beliefs, which Susan may or may not have even shared. Jason Torres chose to do what he believed his wife would have wanted. I've told Mr. Nola that I'd want the same thing if I were pregnant, although we both feel strongly about not remaining on life support if there is no hope. Susan did indeed have hope, maybe not for her own life, but for that of her baby.
That baby has appropriately been named Susan. She made it to 26 weeks gestation and has a pretty good chance of being just fine. I had a box of our Susan's preemie size clothes that I'd been looking for someone to give to, so I shipped it up to the Torres family. May this new little Susan wear them in good health.
Naturally, I've been rooting for this baby. As terrible as the family's loss is, they have Susan's last great gift to the world to remember her by. My own Susan, as well as many other preemies, are testaments to the quality of life that is possible for kids born early. So it's surprised me to see a lot of people whose opinions I respect criticize Jason Torres, Susan's husband, for keeping her alive. He's been accused of using his dead wife as an incubator, of taxing the medical system's resources for a child with poor prospects, and of neglecting his older child's needs while attending to his dying wife and nascent baby.
On the other hand, he's also being held up as a hero to the pro-life movement, and Susan it's martyr. I'm totally appalled that people are using this family's tragedy to highlight their political beliefs, which Susan may or may not have even shared. Jason Torres chose to do what he believed his wife would have wanted. I've told Mr. Nola that I'd want the same thing if I were pregnant, although we both feel strongly about not remaining on life support if there is no hope. Susan did indeed have hope, maybe not for her own life, but for that of her baby.
That baby has appropriately been named Susan. She made it to 26 weeks gestation and has a pretty good chance of being just fine. I had a box of our Susan's preemie size clothes that I'd been looking for someone to give to, so I shipped it up to the Torres family. May this new little Susan wear them in good health.
Friday, July 29, 2005
Some people are just jerks
Did you see this story about the T-Ball coach bribing a kid to bean a disabled kid on the team, so he wouldn't be able to play? Oh, where to begin. Obviously this guy is a total failure as a human being to place winning a T-Ball playoff game over the safety of a child, any child. I'm ever more bothered that the league has NOT suspended him from coaching pending investigation. Only if he's CONVICTED of assault will they take away his position of influence over other kids.
What the hell? The jerk has admitted to trying the same thing on an umpire in an earlier game. Wouldn't even that be enough to show he's not a good sportsman or role model? And why on earth are the playoffs in T-Ball anyway? Why do they even keep score during T-Ball? It's not about the kids. It's just a way cretins like this guy can compensate for whatever in their lives is lacking.
The autistic boy is probably happy to just get to be on the field with the other kids. And why shouldn't he be there? Because he makes people uncomfortable, or because he might bring down their score? I can just imagine what it took for the mother of this child to get him into the league, to get him to the practices and games and to find a way to participate without being disruptive. I imagine the other parents treating her with either pity or contempt. Frankly, I hope she sues the league for endangering her son.
What the hell? The jerk has admitted to trying the same thing on an umpire in an earlier game. Wouldn't even that be enough to show he's not a good sportsman or role model? And why on earth are the playoffs in T-Ball anyway? Why do they even keep score during T-Ball? It's not about the kids. It's just a way cretins like this guy can compensate for whatever in their lives is lacking.
The autistic boy is probably happy to just get to be on the field with the other kids. And why shouldn't he be there? Because he makes people uncomfortable, or because he might bring down their score? I can just imagine what it took for the mother of this child to get him into the league, to get him to the practices and games and to find a way to participate without being disruptive. I imagine the other parents treating her with either pity or contempt. Frankly, I hope she sues the league for endangering her son.
Thursday, July 28, 2005
Evidently I'm not the only one
Wow. Two days after starting this blog, an internet buddy pointed me to THIS ARTICLE in Brainchild Magazine about the exact.same.thing.
The author's pregnancy and NICU experience were very much like mine. To the extent that I thought, damn, I wish I wrote that! Her son is older and has different issues than Susan, but her feelings about the stress of a sick child and the lameness of the Holland analogy were my own.
I think the folks who hand the Holland story to someone with a premature baby are just displaying what I've found to be a common romanticizing of the disabled and the carers for the disabled. We're all supposed to be brave, cheerful, and strong in our faith in God. Our kids are supposed to be sweet and affectionate, and if not cute in the traditional sense, cute like that kid from the tv show "Life Goes On." We're supposed to be so grateful to be 'special."
Not that Susan is not in fact gorgeous and funny and affectionate. She is. But her being sick isn't a blessing. Some time last year, when Susan was really sick and I was just despondent with exhaustion, frustration, and fear, I tried telling a close friend about how mad I was that this had happened to us. She said, "But you know you're really lucky, right?" And yes, I am lucky that Susan is alive and doing as well as she is, all things considered. But compared to most new parents, I don't think I could have been called lucky. That's what's so hard. You can't even complain and feel sorry for yourself when you've got every reason to do so, because the rest of the world demands a Pollyanna.
Last night actually went pretty well. We put her on a pump at a lower rate than usual and only had to get up once to vent her at 4 and then again when she woke up at 8. Venting every four hours is totally doable.
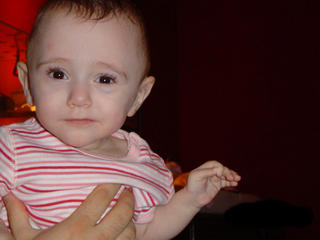
Here's another shot of my spectacular girl.
The author's pregnancy and NICU experience were very much like mine. To the extent that I thought, damn, I wish I wrote that! Her son is older and has different issues than Susan, but her feelings about the stress of a sick child and the lameness of the Holland analogy were my own.
I think the folks who hand the Holland story to someone with a premature baby are just displaying what I've found to be a common romanticizing of the disabled and the carers for the disabled. We're all supposed to be brave, cheerful, and strong in our faith in God. Our kids are supposed to be sweet and affectionate, and if not cute in the traditional sense, cute like that kid from the tv show "Life Goes On." We're supposed to be so grateful to be 'special."
Not that Susan is not in fact gorgeous and funny and affectionate. She is. But her being sick isn't a blessing. Some time last year, when Susan was really sick and I was just despondent with exhaustion, frustration, and fear, I tried telling a close friend about how mad I was that this had happened to us. She said, "But you know you're really lucky, right?" And yes, I am lucky that Susan is alive and doing as well as she is, all things considered. But compared to most new parents, I don't think I could have been called lucky. That's what's so hard. You can't even complain and feel sorry for yourself when you've got every reason to do so, because the rest of the world demands a Pollyanna.
Last night actually went pretty well. We put her on a pump at a lower rate than usual and only had to get up once to vent her at 4 and then again when she woke up at 8. Venting every four hours is totally doable.
Here's another shot of my spectacular girl.

Wednesday, July 27, 2005
You have to love Google
Ha! After yesterday's bitch-fest about Susan's digestive problems, the Google Ad Generator is putting up links for Mylicon and Enfamil AR. Gee, why didn't I think of that? Mylicon, that will solve everything!
When Susan starting eating from the bottle in the hospital she pretty much immediately had trouble. She'd take half the amount she was usually fed by tube and refused any more. Mylicon was the FIRST thing we tried. It works by decreasing surface tension on liquids in the stomach, so small bubbles will pop and gas will form one bib bubble that's easier to burp out. Never worked out for us. I was very disappointed that it wasn't a silver bullet that would allow Susan to start eating normally. It was the first of many such disappointments.
We did leave the pump off last night, and I only got up once to give her a quick feeding. After six uninterrupted hours of sleep, I'm like a new woman. The baby is like a new baby too - her mood is SO much better today than it's been the past week. I guess she suffers from sleeping badly too.
I always have ounces of formula and calories running through my head. At her current weight, Susan needs a minimum of 770 calories a day, or 38 and a half ounces of formula. At night she can take as much as 3 oz/hour on the pump, during the day she only can take about 2 oz/hour. Without the pump, there's just no way, unless I could get her onto a formula that has 30 calories and ounce. So far she hasn't tolerated that at all.
I'm setting up another round of appointments with an allergist, a new gastroenterologist, and a dietician. Maybe we can regroup and get a better plan together.
When Susan starting eating from the bottle in the hospital she pretty much immediately had trouble. She'd take half the amount she was usually fed by tube and refused any more. Mylicon was the FIRST thing we tried. It works by decreasing surface tension on liquids in the stomach, so small bubbles will pop and gas will form one bib bubble that's easier to burp out. Never worked out for us. I was very disappointed that it wasn't a silver bullet that would allow Susan to start eating normally. It was the first of many such disappointments.
We did leave the pump off last night, and I only got up once to give her a quick feeding. After six uninterrupted hours of sleep, I'm like a new woman. The baby is like a new baby too - her mood is SO much better today than it's been the past week. I guess she suffers from sleeping badly too.
I always have ounces of formula and calories running through my head. At her current weight, Susan needs a minimum of 770 calories a day, or 38 and a half ounces of formula. At night she can take as much as 3 oz/hour on the pump, during the day she only can take about 2 oz/hour. Without the pump, there's just no way, unless I could get her onto a formula that has 30 calories and ounce. So far she hasn't tolerated that at all.
I'm setting up another round of appointments with an allergist, a new gastroenterologist, and a dietician. Maybe we can regroup and get a better plan together.
Tuesday, July 26, 2005
Getting a grip
Earlier tonight I was sitting on the couch, head in hands, crying in exhausted frustration as my daughter wailed through the monitor from her bedroom. Her dad was putting her down, as she was just as tired and miserable as we were, and even though she goes to sleep easier if I hold her, at the moment I just could.not.deal.
The poor kid's been sick all day. I've been trying to introduce new foods to her, so I can transition her to a blenderized diet of foods more appropriate to an almost-two-year-old than infant formula. I think I can put "banana" in the not so good category. She threw up five times between noon and two o'clock; spitting out thick mucus while her stomach contracted so hard I could hear it. She's got to have some kind of allergy, but no matter what formula we give her, there's always something that isn't right. Everything we've tried - soy, lactose-free, elemental, metabolic, organic, yadda yadda - gives her some degree of indigestion that presents itself with gas, mucus, constipation, or projectile vomiting.
We've been at a pretty good equilibrium for the past six months, having found completely by accident that she does much better on liquid than powdered formula. Still, we have had to vent gas from her stomach though her g-tube on a nearly hourly basis around the clock. The last time I slept an entire night was when I went on vacation in April. On a day by day basis, it's not so bad. I can nap with the baby during the day, and at night I go back to sleep easily after getting up about every two hours. Over months though, I'm wearing down. And I'm starting to feel that this is just ridiculous. This can't be normal can it? Even for a kid with reflux and a g-tube?
Everything is a trade-off. We could get more sleep if we didn't feed her at night, using a pump to deliver formula through the g-tube, but she gets most of her calories during that time. It's been such a struggle to get any weight onto her I can't imagine giving that up. Maybe just for tonight.
The poor kid's been sick all day. I've been trying to introduce new foods to her, so I can transition her to a blenderized diet of foods more appropriate to an almost-two-year-old than infant formula. I think I can put "banana" in the not so good category. She threw up five times between noon and two o'clock; spitting out thick mucus while her stomach contracted so hard I could hear it. She's got to have some kind of allergy, but no matter what formula we give her, there's always something that isn't right. Everything we've tried - soy, lactose-free, elemental, metabolic, organic, yadda yadda - gives her some degree of indigestion that presents itself with gas, mucus, constipation, or projectile vomiting.
We've been at a pretty good equilibrium for the past six months, having found completely by accident that she does much better on liquid than powdered formula. Still, we have had to vent gas from her stomach though her g-tube on a nearly hourly basis around the clock. The last time I slept an entire night was when I went on vacation in April. On a day by day basis, it's not so bad. I can nap with the baby during the day, and at night I go back to sleep easily after getting up about every two hours. Over months though, I'm wearing down. And I'm starting to feel that this is just ridiculous. This can't be normal can it? Even for a kid with reflux and a g-tube?
Everything is a trade-off. We could get more sleep if we didn't feed her at night, using a pump to deliver formula through the g-tube, but she gets most of her calories during that time. It's been such a struggle to get any weight onto her I can't imagine giving that up. Maybe just for tonight.
About Susan
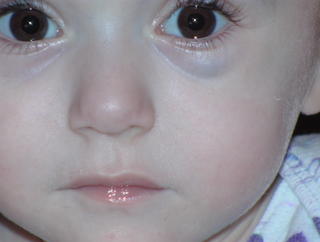
Susan E. came into the world in November of 2003, 12 weeks premature and weighing 15 ounces. Unbeknownst to me at the time, I had a pregnancy complication called pre-eclampsia that caused the blood flow through the umbilical cord to be restricted, limiting the baby's growth. The pre-eclampsia turned into a condition called HELLP Syndrome, where my internal organs began to swell and my blood pressure shot up as my liver started to fail. I was, at the time, 29 years old, healthy, and had no reason to expect any trouble with the pregnancy.
When the shit finally hit the fan, Susan was delivered by emergency cesarean. It was the first of many adjustments I'd make, as I'd always fancied myself the earthy, granola, natural birthing type. Suddenly instead of being six months pregnant I had a scar on my belly and a tiny, writhing, REAL little person with my name written on her identity card.
She was, and continues to be, a survivor. 95-98% of babies born weighing less than a pound have some degree of cerebral bleed, which cause brain damage. She did not. Nor did she develop an ulcer, or a heart defect, or retinal detachment, or "gut rot," or many of the really bad complications of prematurity that could have threatened her survival. She did spend five and a half months in the hospital, many weeks on a ventilator, suffering damage to her lungs and many painful procedures. She never successfully learned to eat from a bottle, so we reluctantly agreed to have a g-tube inserted in her stomach so we could take her home.
Over the next year at home, she has amazed us all. She is funny, engaging, and stubborn. As far as we can tell, her mental development is coming along fine. She is however, held back by physical growth. Her oral feeding deteriorated as she developed uncontrolled reflux, vomiting after every tube feed, and she refused anything in her mouth but her one, precious, pacifier. Her weight crept up, or plateaued at times, but she has remained far below growth curve.
Her gross motor skills are significantly delayed. At 20 months, she doesn't walk or pull to a stand. She won't crawl, but she scoots around very efficiently. I think her lack of crawling is more stubbornness than anything else. Her fine motor skills - reaching, grabbing, using her hands - are quite good. Since talking uses the same musculature as eating, her speech is delayed. She babbles, but is not using words yet. Feeding is a long, hard skill to learn for someone who didn't get it in the first place. She is making progress, but it will be a long time before we can take our her g-tube.
Updating this, since about two years have passed since it was written -
Susan's almost 4. She is like any three-year-old in most ways: she is funny and cute, has a passion for Clifford the Big Red Dog, walks, climbs on the playground and throws embarrassing tantrums at Target. Her speech is delayed, but making rapid progess. She can identify objects and speaks in short sentences. She reads along with her favorite books, having memorized the words.
Eating continues to be a challenge, but she's made such great progress. She can eat smooth foods like yogurt. We regularly puree whatever we're eating and feed her that orally, and (diluted) through the feeding tube. She hasn't figured out chewing yet, so solids either get spit out or she keeps them in her mouth long enough that they dissolve. But she'll put anything into her mouth, and hardly ever gags anymore. It's huge.
She's still TINY. No matter how much food I pump into her, she'll get taller but not wider. At almost four, she's about the weight of a typical 15 month baby, although her height is on the low range of normal.
Subscribe to:
Comments (Atom)
